This is a sequel to my previous post talking about stubborn peri-menopausal and menopausal bulge, where I outline how the bulge can be attributed to hormones-not only sex hormones but insulin as well. Click here to view that post.
In this post we’ll take a deeper dive into how to identify insulin resistance and the strategies to implement to become more insulin sensitive.
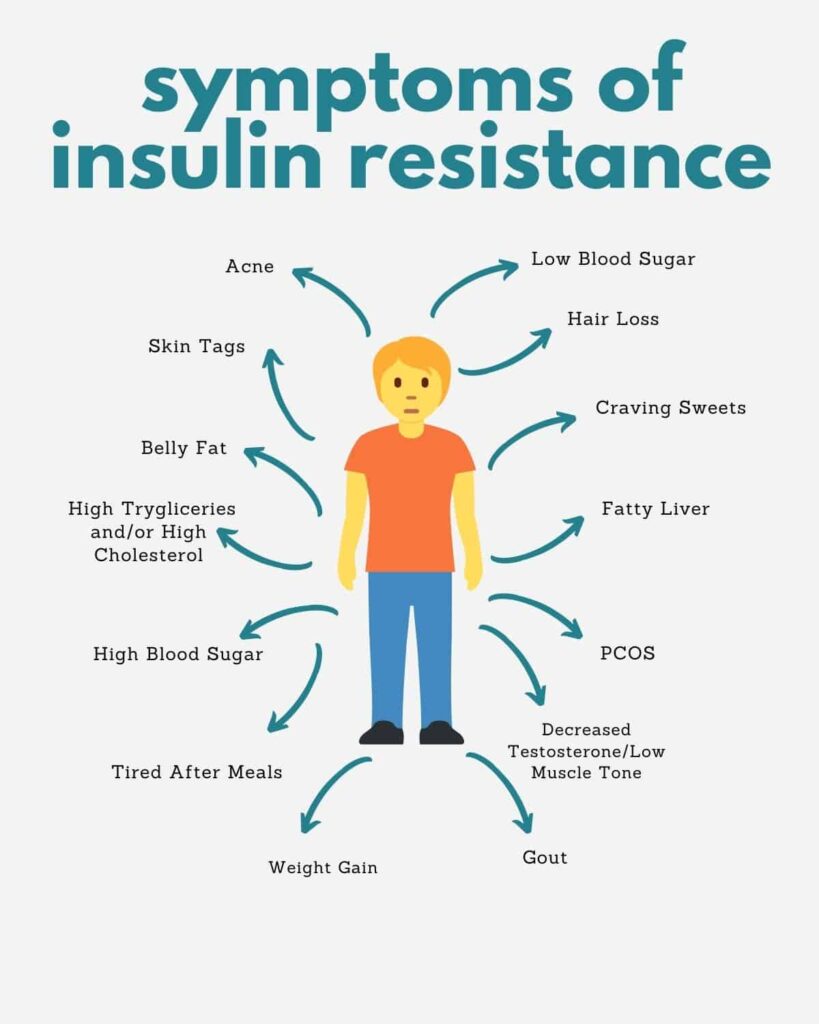
Physical signs of insulin resistance include:
· Fatty Liver
· Weight Gain in the middle
· Skin tags
· Darkening of the skin in armpits and around the neck
· HBP
Now, just to be clear, you can have insulin resistance without having these physical signs but if you do have these signs, it’s very likely you have insulin resistance.
Blood tests that suggest (but not diagnose) insulin resistance include-Elevated
· Triglycerides
· Cholesterol (which of course, means that reversing insulin resistance can be an excellent way to lower cholesterol- (reaching for a statin is most often not the answer)
· Liver enzyme ALT
· C-reactive protein (CRP)
· Low HDL
Sometimes, blood glucose and HbA1c can be high as well. But quite often glucose and HbA1c are normal with mild to moderate insulin resistance. Which means that if your doctor only tested for glucose or HbA1c, which is where most doctors stop, then they did not test for insulin resistance!
The easiest way to test for insulin resistance is with a simple fasting insulin test done through blood work. More than likely, you will have to ask for it. It’s not something doctors are trained to test. Why? Because there is no drug that lowers insulin levels…
A more comprehensive test and gold standard is the glucose tolerance test with insulin. This is a challenge test to see how your body handles a very sugary drink measuring BOTH glucose and insulin levels at different intervals-before and after ingesting the drink.
A healthy fasting insulin should be less than 8 mIU/L. One and two hours after the glucose challenge, a healthy insulin should be less than 50 mIU/L. Of course, it’s normal for insulin to rise after the glucose challenge and after a meal. That’s its job. And insulin at the right level has many benefits including modulating circadian rhythm, building muscle, and if you’re a young woman, keeping your period going.
Insulin that is above these reference ranges—either fasting or peak insulin is a problem. High insulin is a driver of weight gain, disease, and metabolic dysfunction, and a biomarker of underlying cellular dysfunction (aka aging).
But the good news is that it’s reversible! As insulin sensitivity improves, and insulin comes down, metabolic function is restored and weight loss can occur. In general, it’s probably not possible to lose much abdominal weight, or abdominal fat, until fasting insulin comes below 8 mIU/L, which can take several months depending on how high insulin was to start with.
But the thing to understand is that you could be achieving significant metabolic improvement, ie. reversing insulin resistance, for weeks or even months before you notice significant weight loss. Which means you should not get discouraged if you don’t lose weight right away. As long as your insulin is coming down-you’re good! Insulin coming down means your metabolism is improving and you are setting yourself up for better health and future weight loss.
Insulin resistance is a little complicated but it’s basically when the mitochondria (the energy powerhouses in our cells) are overwhelmed by energy excess or other insults and they signal the rest of the cell including the insulin receptors to stop responding to insulin. This temporarily stops the flow of glucose to the mitochondria (because they can’t handle anymore glucose) and temporarily shelters the mitochondria.
So, what causes the mitochondrial distress and therefore insulin resistance in the first place? It’s a big question and the answer is lots of things including energy excess aka overeating but other things as well.
Other insults to mitochondria and insulin sensitivity include:
· Environmental toxins
· Medications
· Ultra-processed food
· Circadian disruption
· Muscle loss
· Nutrient deficiency
· Chronic inflammation
· Mouth infections
· Gut issues
—just to name a few.
Below are strategies to reverse insulin resistance. Of course, you don’t have to employ all the strategies at the same time, especially not all the supplements. It’s just a quick overview of some of the things that can work.
Here we go. Effective, evidence-based strategies for reversing insulin resistance include:
· Moving the body to build muscle.
· Eating enough protein.
· Avoiding ultra-processed food, sugars and white flour
· Avoid the consumption of fruit juices (not fruit)
· Fixing any underlying gut problems as inflammation from the gut can cause or worsen insulin resistance.
· Supporting a healthy circadian rhythm with morning light and protein.
· Eating at the same time every day, which also helps circadian rhythm.
· Getting enough sleep.
· Reducing stress and enhancing parasympathetic tone and heart rate variability with breath.
· Boosting oxytocin by, for example, getting a massage or spending time with friends.
· If you’re a woman, maintain adequate levels of estrogen and progesterone, which enhance insulin sensitivity.
· If you’re a man, maintaining adequate levels of testosterone increases insulin sensitivity.
Other strategies include:
· Gentle intermittent fasting, especially fasting overnight, which is called time-restricted eating-12 hours.
· Supplements such as magnesium, taurine, myo-inositol, berberine, silymarin, and choline. Silymarin and choline work primarily by improving fatty liver.
So that’s the skinny (pun intended) on how to identify and treat/manage insulin resistance.
I hope this has been helpful!
If you’d like to schedule an introductory call with me please click HERE.